Traumatic Brain Injury Diagnosis
Health care providers usually diagnose a traumatic brain injury (TBI) using a combination of medical history and neurological exams. Imaging studies, such as a CT scan or MRI, may also be used, particularly in cases of severe TBI. Although immediate evaluation is recommended after any head injury, it’s possible for the diagnosis of a TBI to be made months or even years after the injury.
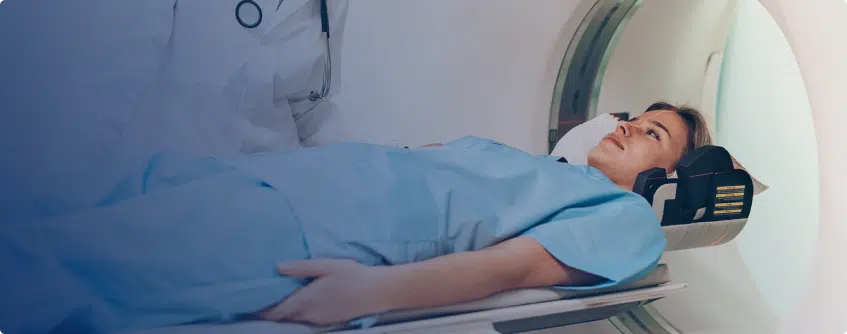
After a person experiences a head injury, doctors will need to perform an evaluation to determine whether they have a traumatic brain injury (TBI). The process of diagnosis begins with a medical history and neurological exam. Imaging studies, like a CT scan or MRI, may also be used, although they’re not always necessary.
Early diagnosis of a TBI, whether a severe traumatic brain injury or a mild injury can be lifesaving. Doctors will look for signs of skull fractures, bleeding inside the skull, contusions and hematomas, blood clots, hemorrhages, memory loss, blurred vision and other complications.
How are traumatic brain injuries diagnosed?
After a head injury, doctors use a variety of different methods to evaluate a patient’s brain function and check for TBI. The first step is a medical history. The doctor will learn as much as possible about the injury to determine what types of injuries are likely to have occurred.
The next step is a neurological exam. Neurologists conduct a thorough medical exam that checks a variety of different functions, including sensory function, body and eye movements, coordination, reflexes, and thinking.
If a patient’s injury appears to be severe enough, then doctors may use imaging studies. The doctor’s clinical judgment ultimately determines whether this is necessary, but the following groups are more likely to get an imaging study:
- Patients who have significant impairments in their nervous system function
- Patients who are vomiting
- Those who have lost memory of a significant period of time around the injury
- Those who are very young or old, including infants, as well as those older than 65
- Those who were intoxicated at the time of the injury
The types of imaging studies that may be used as part of the diagnosis of TBI include:
- Computerized tomography scan (CT scan). This uses X-rays to create an image of the skull and brain.
- Magnetic resonance imaging (MRI). This uses strong magnets to create a detailed image of the brain.
The purpose of neuroimaging immediately after a head injury is primarily to determine whether the patient needs emergency medical care. For example, if there’s evidence of bleeding inside the skull, then a surgical procedure to relieve the intracranial pressure may be urgently needed to prevent severe brain damage or even death. An MRI takes longer, while a CT scan can be performed quickly, making it a better option in the early phases of treatment.
An MRI may be performed later on, sometimes days or even weeks after the injury. The Radiological Society of North America notes that MRIs can detect changes in the brain that CT scans may miss, which can make them useful for evaluating patients who are continuing to experience symptoms from their TBI but whose CT scans are normal.
A study in the Annals of Neurology found MRIs performed soon after the injury may be a useful predictor of outcomes from TBI. Because of this, it may become more common for MRIs to be performed earlier in the course of treatment for a TBI.
The diagnosis of a TBI doesn’t necessarily require a CT scan or MRI. In fact, many mild traumatic brain injuries can’t even be seen in imaging studies. If a patient has experienced a head injury, such as a skull fracture, and is experiencing symptoms consistent with a TBI, then imaging studies may not always be considered necessary to diagnose TBI.
How is the severity of a brain injury measured?
The most common way to measure the severity of a brain injury is using the Glasgow Coma Scale (GCS). This method evaluates the patient’s level of consciousness based on three factors.
- Eye-opening: scored from 1 to 4. A score of 1 means that the patient doesn’t open their eyes at all, while a score of 4 means that the patient spontaneously opens their eyes.
- Verbal responses: scored from 1 to 5. A score of 1 means that the patient doesn’t give any verbal responses at all, while a score of 5 means that they’re oriented.
- Motor responses: scored from 1 to 6. A score of 1 means that the patient doesn’t move the body at all, while a score of 6 means that they can move appropriately in response to commands.
The three scores can be added together to give a total GCS score from 3 to 15. This can be used to classify the severity of a patient’s TBI.
- GCS 13 to 15: mild TBI
- GCS 9 to 12: moderate TBI
- GCS 3 to 8: severe TBI
A patient’s GCS in the early phase of the injury can be used to predict their outcome. Patients with a lower GCS are more likely to die or to have a lasting disability, while those with a higher GCS are more likely to make a full recovery. However, while the GCS can make a prediction of the most likely outcome, it’s never possible to know ahead of time what a particular patient’s course of recovery will be like. Some patients with severe TBI are able to recover well.
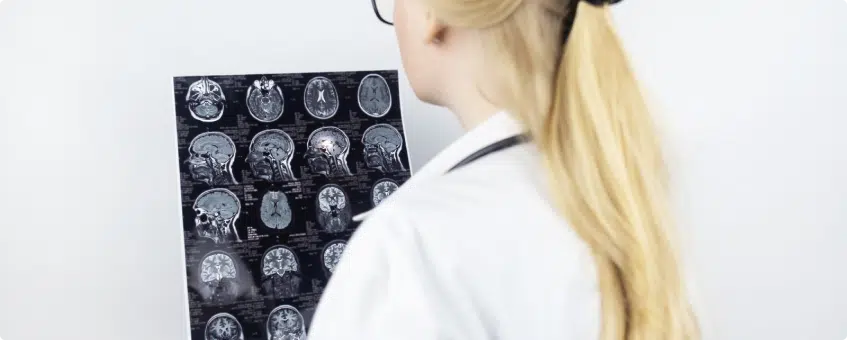
Can a traumatic brain injury be diagnosed years later?
In some cases, it may be possible for a TBI to be diagnosed years later. A TBI can cause lasting changes to the brain that can potentially be detected for the rest of the person’s life.
Some patients are not aware of the changes in their brain function after a TBI, but these may still be detectable through testing, as noted by researchers from The National Institute for the Rehabilitation of the Brain Injured. A neurological exam may find changes in the function of the nervous system that suggest a past brain injury. For example, there may be visual changes, areas of numbness or muscle weakness, or difficulty with cognitive function.
An imaging test of the brain, such as a CT scan or MRI, may be used to confirm that the patient had a brain injury in the past. When brain tissue dies, it’s not replaced. Brain cells don’t divide, so brain cells that are gone are gone forever. The dead tissue will be reabsorbed by the body, leaving a change in the appearance of the brain that may be visible many years later.
A patient’s symptoms, including memory problems, confusion, and blurred vision, along with a neurological exam and imaging studies may show that there was damage to their brain in the past, but it won’t necessarily be able to pinpoint the cause of this damage.
For example, brain damage from a TBI or a stroke could look much the same many years later. If the patient remembers sustaining an injury, this could be helpful in determining the cause of the past brain damage.
Even though lost brain cells will not grow back, this doesn’t mean that it’s impossible for a person to recover the functions of the lost areas. The brain is extremely flexible, and other parts of the brain may be able to change their functions to make up for the parts that have been damaged by the injury.
What methods are used to screen for TBIs?
There are a few different screening tools available that can be used to check for evidence of a past TBI that’s still causing symptoms.
For example, the Brain Injury Screening Test (BIST) asks people whether they’re having a variety of symptoms, including headaches or neck aches, trouble with memory or concentration, problems sleeping, mood changes like irritability, visual disturbances, or excessive sensitivity to bright lights.
The more of these symptoms a patient has, the more likely they have experienced a past TBI. Neurological symptoms like these could have a variety of different causes, so the screening test also asks people whether they’ve ever hit their head to determine whether a TBI is a possible explanation for their symptoms.
A study in the Journal of Head Trauma Rehabilitation showed that about 9 percent to 12 percent of non-high-risk participants reported “a history of TBI with chronic symptoms” on the Brain Injury Screening Questionnaire used for the study. Of the participants classified as high-risk, 27 percent to 54 percent reported TBI with chronic symptoms. The high-risk participants included college athletes, people experiencing homelessness, and people who were in the justice system.

When to contact a doctor
Many people, unfortunately, avoid seeking treatment after a head injury. This may be due to embarrassment, especially if the injury was caused by a fall in one’s own home. Often, people also underestimate the damage that a TBI can cause and decide that the severity of their head injury doesn’t require medical care.
However, it’s important to seek treatment for any head injury, even if the injury appears to be mild. This allows your doctor to screen for signs that the injury may be more serious than it seemed. It also ensures that you get medical advice about how to take care of yourself after the injury, along with any treatments that you may need to maximize the chances of a good recovery. If you’ve experienced any bump, blow, or jolt to the head, you should see your health care provider as soon as possible to be evaluated.
After a head injury, if you experience any of the following concussion symptoms, you should seek emergency medical care right away:
- Severe headache
- Vomiting repeatedly
- Difficulty using your arms or legs
- Worsening sleepiness or confusion
These are signs that pressure may be building up inside your skull. Without prompt treatment, this could cause severe and permanent brain damage and could even be fatal. If you’re with someone who has recently experienced a head injury or loss of consciousness and displays these signs, get them to the emergency room right away.

$4,500,000
Recovered for a client who sustained a traumatic brain injury in a car crash.
DO I HAVE A CASE?
If you think you may have a TBI case, contact us now for a FREE consultation